Recovery from torn retina surgery6/30/2023  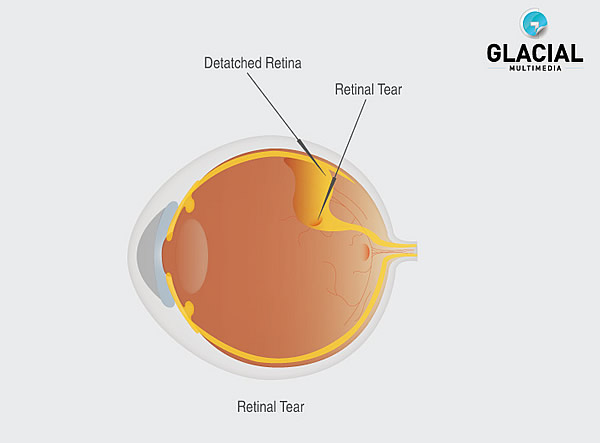
Protective shield should be worn for at least a week and guidelines should be followed closely to ensure incisions heal properly without disruption. Activity must be restricted, and patients should refrain bending and heavy lifting (2-10 lb. They are important for preventing inflammation and bacterial infections. All patients must take postoperative drops. Patients are encouraged to rent the face down apparatus that will help with face down positioning. For those who have been treated with a gas bubble, proper face down positioning is imperative to reinforce the retina and help it heal properly. In order to have the best possible outcome after surgery there are several things to keep in mind. The gas is used to hold the retina in place while either the laser or freezing can work. Pneumatic retinopexy: A gas bubble is injected into the vitreous along with a combination of laser or freezing around the tear. Allow 4-6 weeks for proper healing time following these treatments. Freezing is used with a special probe that applies intense cold to freeze the retina resulting in scar tissue that will help encircle and fully seal the tear. The burns result in scarring that aids in sealing of the tissue around the tear, which prevents fluid from progressing and leading to a full blown retinal detachment. Laser/ Freezing treatment: Your surgeon will perform laser to make small burns around the tear. 
The fluid under the retina is drained from the outside, and freezing treatment is applied to the break to seal it. This is done by placing an encircling buckle around the eye and tightening it. The point of the scleral buckle surgery is to try to relieve the traction placed on the retinal break by moving the wall of the eye inwards. Scleral Buckle: A scleral buckle surgery is performed from the outside of the eye, in contrast with the previous vitrectomy surgery where instruments were introduced in the middle of the eye. Lastly, either gas or oil is placed in the middle of the eye, allowing the retina to be pressed up against the back of the eye until the laser heals. Care is taken to completely encircle any existing breaks. Once the retina is flattened, 360-degree laser is performed to ensure the peripheral retina is well tacked down. 
The fluid is then removed from under the retina. 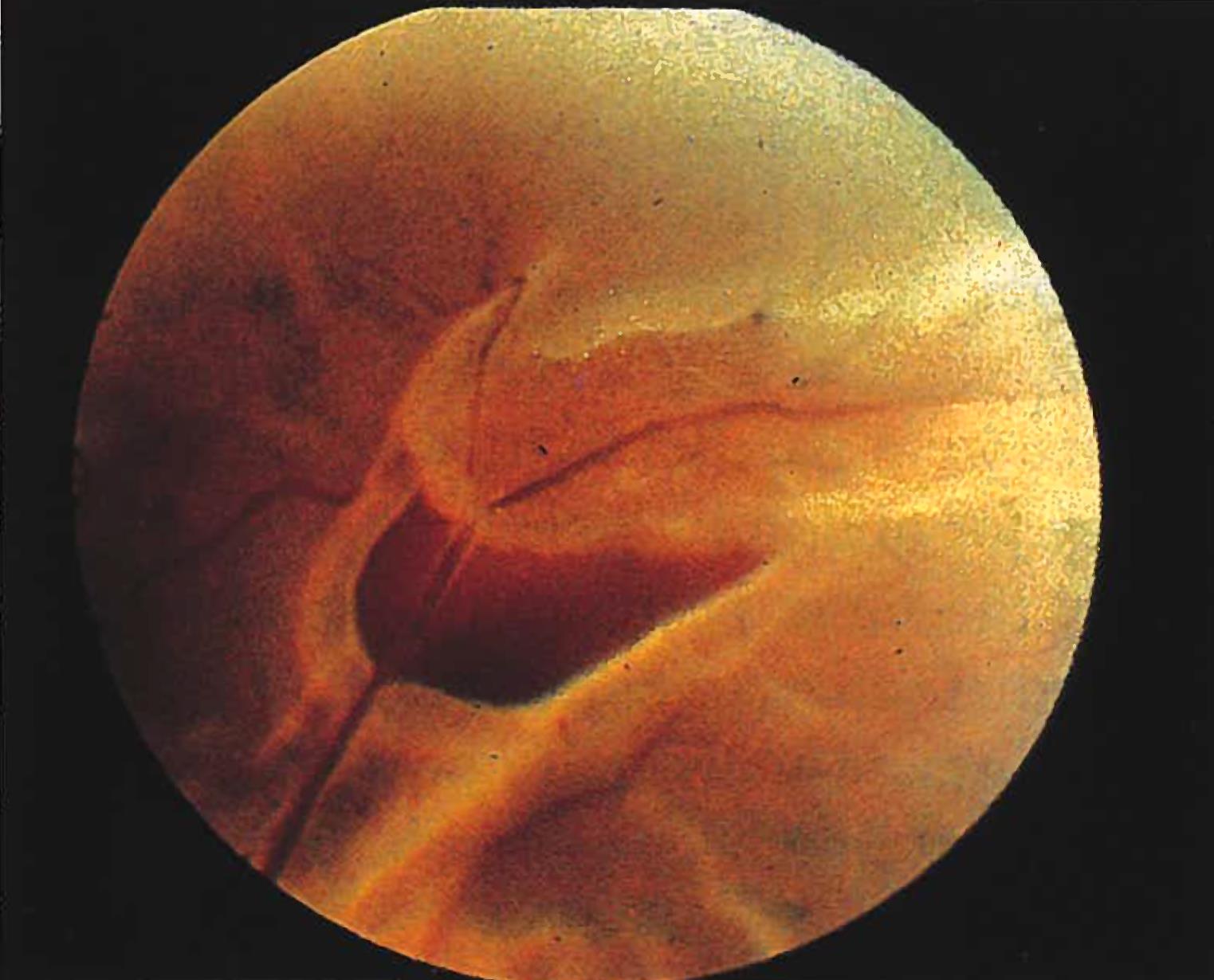
The vitreous gel is removed, taking care that any traction on the existing tear is released. During this procedure, a surgeon makes small openings in the sclera through which instruments can be inserted into the eye. Vitrectomy: A detachment may be repaired by several different surgical procedures. Proper reattachment of the retina is important in order best preserve your vision. The choice in procedure will be picked based on the type of retinal detachment you have and your specific situation. There are many ways to successfully repair a retinal detachment. If not treated in a timely manner a retinal detachment may lead to permanent vision loss. The liquefied vitreous goes under the retinal tear and accumulates behind the retina causing a retinal detachment. This pull can cause traction on the retina, resulting in a retinal tear. The most common way retinal tears occur is through a normal aging change where the vitreous – a clear jelly like substance – pulls loose and separates from the retina. Often, retinal detachments occur after a retinal break or tear. The retina is made up of several regions - the macula which is responsible for detailed pin- point central vision and the peripheral retina which is responsible for your peripheral vision. When light enters our eyes through the cornea and lens, the image is focused on the retina. The retina is very thin, light sensitive tissue that lines the back of the eye. Tips to fasten recovery after surgery for Detached Retina 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
